 Syphilis (congenital and acquired) (8, 19).There are some systemic infections and inflammations that have been reported to cause a tonic pupil, which includes the following (8): Optic nerve sheath fenestration (especially lateral orbitotomy approach) (12)Ĭiliary Ganglion Injury Associated With Systemic Illness.Ocular and orbital surgeries that have been associated with ciliary ganglion injury include the following (8): The ciliary ganglion can be injured directly or iatrogenically. When in association with a loss of deep tendon reflexes (hyporeflexia or areflexia), it is called Holmes-Adie syndrome (8). Other clinical features include segmental iris sphincter palsy, light-near dissociation, and cholinergic hypersensitivity. The denervation occurs at the level of the ciliary ganglion, with aberrant regeneration of accommodation occurring over the course of the next 1-2 years. Adie's tonic pupil is typically initially unilateral (80%), with increased risk of involvement of the contralateral pupil over time. This results in a sudden fixed, dilated pupil and loss of accommodation in that eye. They eventually merge with the nasociliary nerve (V1), which travels through the annulus of Zinn.Ĭlinical Correlations Adie's Tonic Pupil and Holmes-Adie Syndromeįor more information about Adie's pupil, stay tuned - I plan to write a separate article (or more) about the subject.Īdie's tonic pupil is characterized by an idiopathic, sudden-onset denervation of the ciliary body and iris sphincter, followed by a slow abnormal reinnervation. The sensory nerves travel along both short and long ciliary nerves.Keep in mind that some of the sympathetic nerves will also travel along the short ciliary nerves. The postganglionic sympathetic nerves travel a long distance from the superior cervical ganglion to get to the eye and travel along the long ciliary nerves.The postganglionic parasympathetic nerves have a short distance to go to the eye and travel along the short ciliary nerves.Only 1 group of nerves synapses in the ganglion (parasympathetic).There are essentially 3 groups of nerves that course through the ciliary ganglion (sensory, parasympathetic, sympathetic).These sympathetic fibers do NOT synapse in the ciliary ganglion, and follow the long posterior ciliary nerves and short ciliary nerves to innervate the pupillary dilator muscle (1-2, 6) Tips and Hints These are NOT myelinated, and arise from the superior cervical ganglion, which is located near the angle of the jaw and the bifurcation of the common carotid artery. There are also postganglionic sympathetic fibers that course through the ciliary ganglion. They course along the short ciliary nerves to innervate the iris sphincter (only 3-5% of the postganglionic parasympathetic fibers are pupillomotor!) and ciliary muscles (6-7). The postganglionic (postsynaptic) parasympathetic nerves are myelinated. These fibers course along CN3, follow along the inferior division of CN3 when it splits at the level of the annulus of Zinn, and forms the motor root entering the ciliary ganglion, where they synapse. As you might guess, the parasympathetic fibers here mediate the pupil constriction (light) and accommodative responses. 
Preganglionic (presynaptic) parasympathetic nerves arising from the Edinger-Westphal nucleus in the CN3 complex synapse in the ciliary ganglion. These fibers travel along the short and long ciliary nerves through the ciliary ganglion without synapsing and forms a sensory root exiting the ciliary ganglion posteriorly before merging with the nasociliary nerve, which course along V1 and ultimately synapse at the trigeminal ganglion (1).įor more information about the sensory nerves to the eye, stay tuned - this will be a separate article. The sensory nerves that travel from the eye are actually fibers of the nasociliary nerve, a branch of the trigeminal nerve (V1). 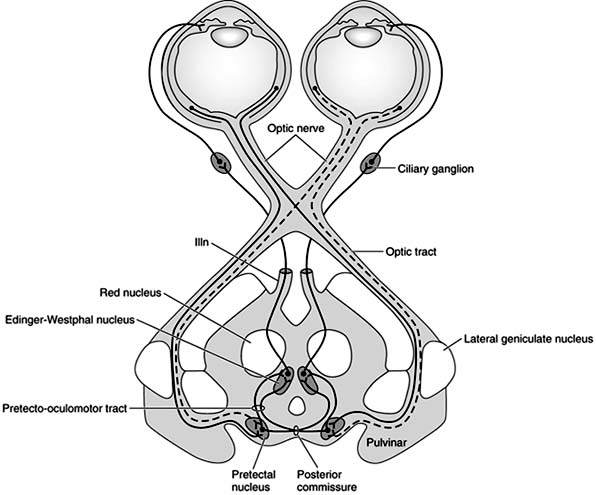
It receives its blood supply from the posterior lateral ciliary artery (supplying the anterior half of the ganglion) and from the lateral muscular arterial trunk (entering the ganglion from its lateral side) (2, 5). 
The ciliary ganglion is small, usually measuring 2 mm horizontally and 1 mm vertically. According to the Basic and Clinical Science Course, it is located lateral to the ophthalmic artery, situated between optic nerve and lateral rectus muscle, approximately 1 cm (10 mm) anterior to the annulus of Zinn and 1.5-2 cm (15-20 mm) posterior to the globe (1-5). Because of the many nerves that course through it (not all of them synapse!) and its anatomical location, this structure is of importance in learning the basics of ophthalmology. The ciliary ganglion serves as the site of synapse for the parasympathetic nerves innervating the eye. 
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
